
| Home |
| Dynamics of Pharmaceutical Care: Developing Collaborative Working Relationships Between Pharmacists and Physicians [J Am Pharm Assoc 41(5):682-692, 2001. © 2001 American Pharmaceutical Association, Inc.] |
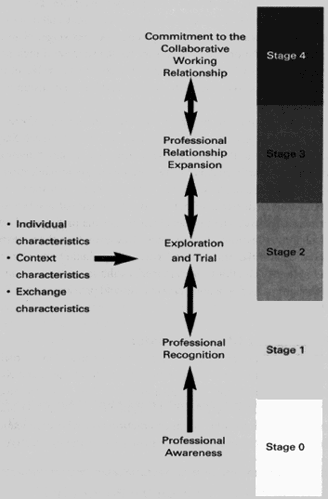
Figure 1. Staged Approach to Developing the Pharmacist-Physician Collaborative Working Relationship
Figure 2. Patient Agreement Form
ANTICOAGULATION MONITORING PROGRAM
A Pharmacy X Clinic Pharmacy Program
COLLABORATIVE CARE AGREEMENT
Physician's Name:___________________________________
Office Address:_____________________________________
Phone Number:______________________________________
Physician's UPIN:_____________________________________
I am aware that there is a collaborative care agreement between _____________________________________________ (Physician) and ________________________________________ (Pharmacist) to manage my anticoagulation, including adjusting my anticoagulant dose, ordering lab tests, and scheduling follow-up appointments. I also understand that I will be informed immediately of any changes in this agreement.
Patient's Signature_______________________ Date________
Pharmacist's Signature____________________ Date________
___________________________________________________
UPIN = Unique Physician Identification Number.
Figure 3. Collaborative Practice Agreement Form
ANTICOAGULATION PROTOCOL
A Pharmacy X Clinic Anticoagulation Program
Management by Pharmacy X Clinic Pharmacies
- Pharmacy X pharmacists will complete lab orders and coordinate the draw (fingerstick) to fit the patient's schedule.
- Patient will be assessed for bleeding/bruising, missed or extra doses, alcohol use, compliance, drug changes, diet changes, health changes.
- Warfarin Dosage
- Appropriateness for warfarin dosage is assessed based upon INR within the context of compliance, patient's anticoagulation history, possible interactions, and complications.
- Dosage of warfarin is adjusted as necessary. The agreed-upon protocol will be followed.
- Small dosage adjustments are made.
- For high INRs: assess compliance, drug interactions, diet changes, and alcohol consumption, then recheck lab, hold doses, use vitamin K, decrease dose, or contact supervising physician based on patient clinical status.
- For low INRs: assess compliance, drug interactions, and diet changes, then recheck lab, start medication, increase dose, or contact supervising physician based on patient clinical status.
- Patient and/or caregiver is advised of the dosage change and the new dose is written down for the patient.
Physician's Signature___________________________Date_________
Pharmacist's Signature_________________________Date_________
| Boundary or turf concerns
Communications breakdown Power issues Lack of trust in another practitioner's competence Practice sites distant from one another |
Participant characteristics
Individual characteristicsContext characteristics Proximity of practicesExchange characteristics Attraction |
|
|
|
|
|
|